Living in Texas, where 32% of the population is considered obese, I’ve known quite a few people who have taken a leap of faith and gone under the knife in hopes to save their life. For the most part, many of those individuals have had tremendous success with the procedure. However, there are some who still struggle with their weight.
If you are considering bariatric surgery as an option to help you reclaim your life, then this article is perfect for you.  We cover the history of bariatric surgery, the new and modern options one can choose from, the risks of surgery, and how it requires a change in lifestyle and strict diet. Whether you have always struggled with obesity, or recently found yourself spiraling out of control, there is hope.
We cover the history of bariatric surgery, the new and modern options one can choose from, the risks of surgery, and how it requires a change in lifestyle and strict diet. Whether you have always struggled with obesity, or recently found yourself spiraling out of control, there is hope.
History of Bariatric Surgery
The very first report of bariatric surgery was in 1954, known as the Jejunocolic bypass. Kremen and Linner introduced jejunoileal bypass, the first effective surgery for obesity in the United States, focusing on a mal-absorption bypass theory. Over the course of 50 years, the procedure has undergone numerous modifications and considers the following main techniques as viable options:
- Gastric restriction: Procedure that offers adjustable gastric banding and sleeve banding.
- Gastric restriction with Mild Malabsorption – Combination procedure that provides banding and absorption techniques (Roux-en-Y gastric bypass) as well as the Duodenal switch.
According to the American Society for Metabolic and Bariatric Surgery, the number of patients going under the knife for weight loss is steadily increasing. In 2011, 158,000 people opted in for bariatric surgery, and by 2015, that number grew to 196,000.
Even the amount of males undergoing the surgery has increased over the years, making it, not just a female based operation, but a “health-based” surgery that offers real results to many who continue to suffer from obesity.
Bariatric Options
Nowadays there are several options to choose from when consulting your weight loss options, unlike the first procedure back in 1954. Each option offering their own benefit, risk and lifestyle change.
Gastric Bypass
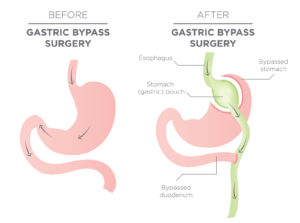
- Considered the Gold Standard of bypass surgery, the Gastric Bypass is broken down into two parts. First, a small stomach pouch is created by dividing the top of the stomach. The second step is to split the small intestine, reconnecting it to the newly formed smaller stomach pouch.
- The process works by leveraging several mechanisms. First, the new stomach is considerably smaller than the original, forcing one to intake less food and calories. Because there is less food to digest, the body absorbs fewer calories and nutrients, thus the malabsorption mechanism. The last mechanism is that by rerouting the food, it changes the hormones produced in the gut to help promote satiety, suppress hunger and contribute to reverse various mechanisms of type 2 diabetes.
- Advantages
- Long Term Weight Loss
- Food Restriction and Intake Control
- Increased Energy Use/Calorie Burning
- Gut Hormone Modifications
- Disadvantages
- More complex than AGB or LSD and greater risk of complications
- Potential long-term vitamin and mineral deficiencies.
- Longer hospital recovery stay
- Strict dietary recommendations, vitamin and minerals supplements and follow-up appointments are mandatory.
Sleeve Gastrectomy
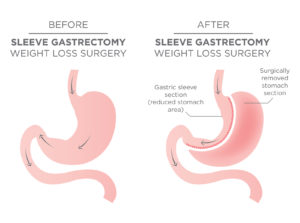
- The Laparoscopic Sleeve Gastrectomy, otherwise known as the “sleeve” is a procedure that removes roughly 80% of the patient’s stomach, significantly reducing the stomach size to about the scale of a banana.
- The procedure first recreates the stomach to a smaller volume to reduce food intake. Like the gastric bypass technique, this new route also promotes gut hormones, but to a much greater degree helping to curb hunger and control blood sugar.
- Advantages
- Reduced Stomach size restricts food consumption
- Fast and significant weight loss performance
- No foreign objects and no rerouting of the intestines
- Short recovery time
- Positive Hormone changes
- Disadvantages
- Non-reversible procedure; permanent.
- Risk of long-term vitamin deficiencies
- Increase in potential early complication rates
Adjustable Gastric Band
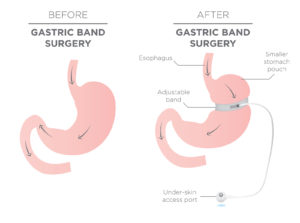
- Similar to the two prior procedures, the adjustable gastric band technique leverages the mechanics of reducing the stomach size. This option utilizes a band that is gradually adjusted over time to further reduce the stomach size and limit the amount of food your body can consume, thus limiting your calorie intake.
- The size of the stomach is maintained by filling the band with sterile saline that is injected through a port placed under the skin. A significant difference between the sleeve and other options is that food is digested and absorbed naturally, meaning there is no malabsorption in this bariatric option.
- Advantages
- Reduction in amount of food consumed
- Substantial weight loss success; 40 – 50%
- No cutting or rerouting of the intestines
- Shorter hospital stays, typically less than 24 hours
- Reversible and adjustable options
- Low rate of postoperative complications
- Low risk of vitamin and mineral deficiencies
- Disadvantages
- Slower weight loss results
- Less efficient than other bariatric options
- Requires a port to remain in the body
- Potential band slippage, erosion or mechanical problems
- Troubles with the esophagus
- Strict diet and frequent follow-ups
- Highest rate of Re-operation
Biliopancreatic Diversion with Duodenal Switch (BPD/DS)
- For short, the BPD/DS is a two-part procedure that creates a small tubular stomach pouch and bypassing a significant portion of the small intestine. The duodenum, or the first part of your small intestine, is divided up just past the opening of your stomach. The distal, or last part, is then reconnected to the stomach opening, creating a way for food to directly empties into the final part of the small intestine. This method bypasses nearly ¾ of the small intestines.
- The bypassed portion of the small intestine is then reconnected to the last part to allow for necessary bile and pancreatic enzymes to take effect on the food eaten. Similar to the other options, BPD/DS does limit the amount of food one can eat, but with time that amount can increase to “normal” amounts of food.
- Advantages
- Greater Weight Loss during five years follow up
- Allows for gradual increase in “regular” meal sizes
- Reduction of fat absorption by 70%
- Improved gut hormone changes
- Effective against diabetes
- Disadvantages
- Greater risk of complications
- Longer Hospital recovery times
- Increased risk of protein, mineral and vitamin deficiencies
- Mandatory dietary and supplementation guidelines
As with any weight loss program, you must remember that it will require lifestyle changes. For those who opt in for bariatric surgery, this is no different. Patients must realize that they will have a new dietary restriction. They must also adhere to a strict supplemental regime. Also, one will find that changing their eating habits is just as much of a factor as the procedure itself, meaning that you can’t live off of McDonald’s the rest of your life.
 Like I said, I’ve had many friends make remarkable strides in losing weight, improving their health, and finding happiness through this procedure. So if you are committed to changing your life for the better, living more healthy, and ready to stick to the rigorous dietary and supplemental plans required for this option to be successful, then you are already winning half the battle.
Like I said, I’ve had many friends make remarkable strides in losing weight, improving their health, and finding happiness through this procedure. So if you are committed to changing your life for the better, living more healthy, and ready to stick to the rigorous dietary and supplemental plans required for this option to be successful, then you are already winning half the battle.








Leave a Reply